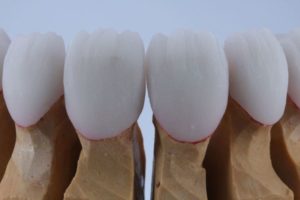
Dr. Lee Ann Brady On Treatment Planning For Peri-Implant Esthetics
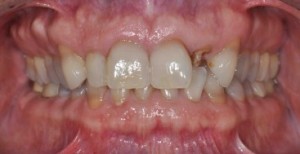 As I complete the series on soft tissue esthetics around anterior implants we have worked our way back to assessing the existing architecture and planning for success. John Kois has simplified the risk assessment process when a natural tooth will be extracted prior to implant placement using five diagnostic keys. I find the thought process invaluable when I plan:
As I complete the series on soft tissue esthetics around anterior implants we have worked our way back to assessing the existing architecture and planning for success. John Kois has simplified the risk assessment process when a natural tooth will be extracted prior to implant placement using five diagnostic keys. I find the thought process invaluable when I plan:
- Tooth Position/Existing Free Gingival Margin: Low risk patients have an existing free gingival margin that is more coronal than the final position, as well as lingually placed teeth. High risk patients have an existing free gingival margin that is apical to where we are proposing for the implant and a facially positioned tooth.
- Gingival Form: Flat gingival architecture is low risk and a high scallop architecture to the existing gingival tissues is high risk.
- Phenotype: Thick tissue type as indicated by not being able to see a perio probe through the gingival tissues when placed in the sulcus is low risk, while thin tissue type creates a high risk situation for optimal peri-implant esthetics.
- Tooth Shape: Square teeth with no existing black triangles are low risk, while triangular or tapered teeth present a high risk situation.
- Osseous Crest Position: Patients with osseous levels coronally positioned on the existing tooth present low risk, while patients with more apically positioned osseous crest are at higher risk of poor pink esthetics after implant placement.
One of the keys to using this system is to follow the evaluation and decision about whether the patients existing conditions are low or high risk in each area. Ask what procedures we can do prior to extraction and fixture placement to reduce the risk and increase the odds of a favorable outcome. This could include orthodontic extrusion of the tooth to be extracted, tissue grafting, and delayed placement of the implant fixture with bone augmentation. Of course, optimal three dimensional placement of the fixture and handling of the hard and soft tissues are always critical.