When Occlusal Instability Presents As Aesthetic Opportunity
Jason Olitsky, DMD, FAACD
When patients present with the desire to improve their smile, for me that is a natural 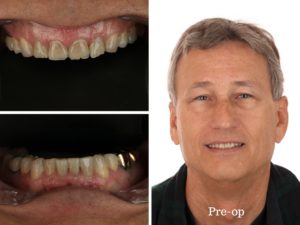 conversation. I love helping patients improve their smiles through a wide range of treatment options including bonding, orthodontics, bleaching, veneers or combination of those modalities.
conversation. I love helping patients improve their smiles through a wide range of treatment options including bonding, orthodontics, bleaching, veneers or combination of those modalities.
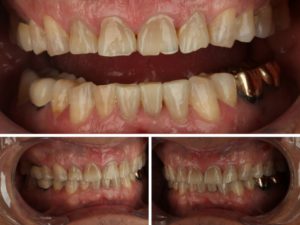
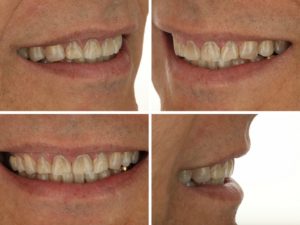
Michael is a patient that was referred by his family and scheduled a consult to see about options for aesthetic improvement. Upon examination of Michael’s teeth, we observed chipping and wear of anterior teeth, as well as excessive wear and restorative breakdown in the posterior teeth from occlusal dysfunction. The lingual patterns and resulting breakdown was indicative of secondary acid erosion.
By determining these risk factors in my initial diagnosis, these factors expand my treatment plan considerations and my conversation with the patient from simply “how to improve the appearance” to “how to make whatever we do last”. The occlusal factors leading to tooth attrition required a thorough evaluation including muscle, activity and joint noise to determine steps required to stabilize his chewing systems. For long-term success, it is essential to treat the patient comprehensively including determining the extrinsic, intrinsic or behavioral reason for the patient’s low Ph.
To start, a full series of radiographs, pictures, videos and clinical exam are first performed and his risk factors are evaluated. We discussed modalities of treatment including discovering the origins of the acidity and uncovering the occlusal disharmony that may exist that contributes to the breakdown of the system. He had been treated with posterior crowns in the past due to wear and fractured back teeth as well as required root canal treatments. He had not had a new cavity in many years.
A key component to communicating the attrition and erosion was to display Michael photographs in our consultation room and have a discussion about findings. This led to co-discovery about habits that may be exacerbating tooth loss, and diet changes that will improve the longevity of any restoration that is placed. In order to adequately plan necessary corrections to the occlusal scheme, evaluating a set of mounted models on an articulator was required assist in developing final treatment recommendations.
After a thorough muscle exam, I determined that a Quicksplint was in order to deprogram the muscles and allow for an accurate centric relation record to be taken in approximately two weeks. The patient was instructed to wear the Quicksplint every night for two weeks, which allows for deprogramming of muscle engrams. I scheduled Michael for a records appointment which includes highly accurate full arch polyvinyl solixane impressions, a Kois face bow record and centric relation bite.
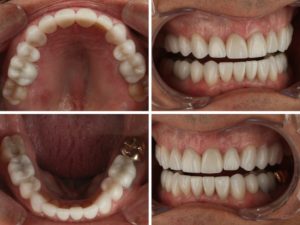
My restorative finding indicated Michael was over-closed and required increasing his Vertical Dimension of Occlusion to gain restorative space and stabilize his occlusion by providing balance in his chewing forces. I prescribed a diagnostic wax up to open the patient to 16mm CEJ to CEJ. I prepped the patient and temporized utilizing the diagnostic wax-up. This allowed Michael some time for his muscles to adapt to the new VDO position, balanced occlusion, try on shapes and sizes intra-orally and report any issues which were none. He was happy and comfortable. After 4 weeks, we inserted 24 e.Max restorations.
So his treatment to improve his smile, turned into a rehabilitation to address the concerns that would provide longevity and predictability in his treatment. Michael accepted restorative treatment on teeth #3-14 and #19-30. He reports that not only is he thrilled with the aesthetic results but his bite has never been so comfortable and natural.
With comprehensive treatment planning, on every case and excellent tools for diagnosis, we are able to provide definitive treatment and recommend ideal treatment. Patients don’t always accept, but when they know the risk and benefits of treatment, I feel satisfied that I’ve honored my commitment to give them all the information they need to make the decision that is right for them.
Have you seen similar cases in your practice? We would love to hear about them in the comments! Read more from Dr. Olitsky, including planning for smile symmetry, smile design techniques: crooked smile and how he balances family while running a successful practice.

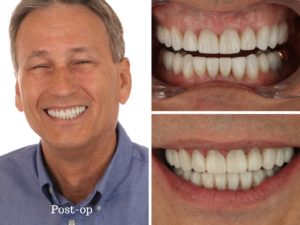

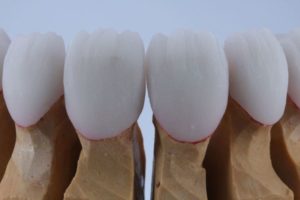

Wow great results Dr Olitsky! 🙂 Couple questions. Looks like he had tetracycline stain. what do you tell the lab to block out the stains? And what cement shade from Variolink LC that you used?
Thank you.
Tam